
Above: Image of a building scaffold. Below: Image of a scaffold structure developed in the lab of Dr. Milica Radisic, University of Toronto. The author has previously written about this structure. Image credit: Raymond Chea (http://news.engineering.utoronto.ca/tissue-velcro/)
 If you live in Toronto (Canada), you know that we have two seasons: winter and construction season. Between new condo developments and homes being renovated or restored, construction is everywhere. Right now, there are five active projects going on in the relatively small neighborhood where I live!
If you live in Toronto (Canada), you know that we have two seasons: winter and construction season. Between new condo developments and homes being renovated or restored, construction is everywhere. Right now, there are five active projects going on in the relatively small neighborhood where I live!
I’m annoyed by the traffic delays and noise pollution, but I’m also aware of all the scaffold structures that are erected around buildings. This is not a coincidence.
Recently, I have been reading and thinking about similar biomaterial structures, also called “scaffolds.” Tissue engineers and biomaterial scientists build different types of scaffolds to be used for regenerating tissues inside of our bodies. I thought it would be interesting to learn more about one type of scaffold developed at Northwestern University. The exciting results of testing these “tissue paper” scaffolds were just published in the Journal of Advanced Functional Materials.
The Extracellular Matrix as an ingredient of building scaffolds for tissue regeneration
In our bodies, all the cells are surrounded by a matrix called the extracellular matrix (ECM). This matrix not only provides a physical base for the cells to stick to, but also plays key roles in organizing the cells into different tissue morphologies, and how they interact with each other, differentiate and maintain the tissue homeostasis. ECM is filled with different proteins and molecules secreted by the cells: such as elastins, laminins, collagens and growth factors.
The ECM is unique for each tissue and has different biochemical and biomechanical components in each organ. This composition changes based on the type of the tissue (for instance liver, bone, or muscle), the physiological state of the tissue (diseased vs. normal), and even the age of tissue. Researchers have spent a lot of time studying ECM since it gives them valuable insights into how the cells interact with each other and what types of environmental cues affect the formation of different types of tissues.
The different components of the ECM have been shown to induce new tissue formation and regeneration. Thus, many biomaterial scientists have tried to create ECM-based biomaterials to be used as scaffolds in tissue and organ engineering techniques. Similar to how in a construction zone the building scaffold structures serve as physical supports and provide accessibility to the different levels that are being repaired or built, the ECM-biomaterial will support and provide the needed substances for tissue regeneration.
A cell free ECM, called a decellularized ECM (dECM), is basically structural proteins of the ECM such as collagen and elastins and bioactive molecules such as growth factors.
A dECM-biomaterial scaffold has a high potential in inducing regeneration and tissue formation, and it does not trigger a host immune response. Also, the ability to design a desired tissue in an in vitro setting makes this scaffold a great candidate for use in various clinical settings.
Decellularizing a whole organ produces dECM; however, due to the scarcity of whole and viable organs, researchers have come up with new methods that use bits of decellularized tissue and mix them directly with a biomaterial that can be readily used for tissue engineering.
The “tissue paper”
Recently, researchers at Northwestern University produced a “tissue ink” that can be used for 3D organ printing projects. Interestingly, an accidental spill of the ink by the lead author of this paper, Dr. Adam Jakus, resulted in his innovative idea of tissue papers. When Jakus tried to wipe the spilled suspension of ovarian tissue and poly-lactic-co-glycolic acid (PLGA), he noticed that it had already formed a sheet structure. This sheet has similar characteristics to paper and it can even be folded into an origami bird, hence the name “tissue paper” or TP. They have used this technique to create different tissue papers from meat and animal byproducts such as heart, kidney, liver, muscle and ovaries.
To make TPs, they crush a tissue that has been stripped off of cells (decellularized) into tissue particles and after further processing they dry it into a powder form. Later, they mix this dECM powder, prepared as shown in the image below, with a solution containing PLGA to make the ink, and let it dry in flat containers to produce the paper.
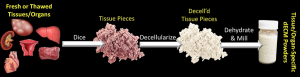
The process of generating dECM powders. Photo credit: Kristin Samuelson, Northwestern University.
Interestingly, the tissue papers had microstructures and topographies similar to the tissues they were produced from. The TPs are mechanically robust and comparatively similar to the original tissue. Muscle TP is stiffer than liver TP for instance. The mechanical properties of TPs also allow them to be manipulated like a paper. For instance, prior to or during surgery, they can be used as bandages to cover a patient’s wound or an internal cut to a tissue.
Each tissue has a certain porosity and ability to absorb fluids and particles; for example, muscle and collagen tissue are less porous than lungs or kidney. The TPs all had porosity profiles relevant to their original tissue. They absorbed liquid while maintaining their structural integrity. This ability is useful for loading them with bioactive molecules, growth factors and antibiotics for treatment purposes.
Also, TPs are biocompatible; they were shown to support the growth of different types of cells in culture. Human stem cells grew on them for up to four weeks, and cell cultures of ovaries on ovarian TPs grew and produced hormones such as estradiol, which plays a role in puberty and fertility. This is really useful since there is a need for biomaterials intended for specific use in reproductive medicine and engineering.
The properties of ovarian TPs were in line with clinical protocols to preserve the tissue to contain a reserve of potential egg cells or oocytes and serve as a source of hormones. According to Teresa Woodruff, one of the principal investigators, this would be really useful for cancer survivors and patients who suffer from infertility or have lost the ability to produce hormones. Strips of ovarian TPs could be planted under the skin to produce puberty hormones or surgically implanted to support the growth of ovarian follicles and restore fertility in cancer survivors.
These tissue papers have huge potential in being used for applications in wound healing and tissue regeneration and repair. According to Ramille Shah, whose lab initiated this innovative idea, “Sky is the limit for where we could use this material alone or in conjunction with the 3D printed materials to create synthetic environments and materials for tissue engineering applications.”
The “tissue paper” is so flexible and thin that Dr. Jakus (the lead author of the original article) has made an origami bird out of it, as you can see in the following video.
Hamideh Emrani
Latest posts by Hamideh Emrani (see all)
- A second chance at life after a diagnosis of Multiple Sclerosis – Day 2 at TMM 2017 - November 16, 2017
- Taming the unruly immune system: the risky stem cell transplant that changed the fate of some Canadian MS patients – Day 2 at TMM 2017 - November 16, 2017
- Ingenious methods to engineer cells to treat diabetes – Day 1 TMM 2017 - November 9, 2017






Comments