If you’ve been feeling like you can’t open a web browser these days without finding a story about induced pluripotent stem cells (iPSCs), you’re not alone. Unlike embryonic stem cells, iPSCs are created by directly reprogramming adult cells taken from donors or patients, and they’ve been all over the news. Most notably, Sir John B. Gurdon and Dr. Shinya Yamanaka were awarded the 2012 Nobel Prize in Medicine last month “for the discovery that mature cells can be reprogrammed to become pluripotent,” and while recent claims that iPSCs had been used to treat heart disease proved fraudulent, the first clinical trials using this type of cell (treating age-related macular degeneration) may begin as early as next year in Japan. [pullquote]…does the public in fact care whether a given therapy uses adult or iPS cells instead of embryonic stem cells? The short answer: Yes, but only under certain conditions.”[/pullquote]Ever since human iPSCs were first successfully produced in 2007, they’ve been touted as a potential “ethical alternative” to human embryonic stem cells (hESCs), since they appear to offer similar benefits to both embryonic cells in general and therapeutic cloning in particular, but dispense with the need to create or harm an embryo in the process. As Condic and Rao note in a 2010 article in Stem Cells and Development:
“[t]he availability of patient-matched, pluripotent stem cells that can be obtained by ethically acceptable means provides important advantages for stem cell researchers, by both avoiding protracted ethical debates and giving U.S. researchers full access to federal funding” [1121]
Pro-life groups have echoed this sentiment, arguing that government funding (in this case, the California Institute for Regenerative Medicine’s grants) should be redirected away from embryonic research and towards work that uses adult stem cells or iPSCs. Indeed, the recent Nobel announcement provided organizations like the Catholic Church the opportunity to reiterate the “superior potential of adult stem-cell research over destructive experimentation on human embryonic stem cells.”
My aim in this post is not to evaluate the relative scientific merits of embryonic versus non-embryonic stem cell research, but rather to consider whether the general public has a preference for iPSCs and adult stem cells. A clear public preference would provide one argument (though perhaps not a very persuasive one on its own) for shifting funding towards non-embryonic research, and would increase the democratic legitimacy of any such change in policy.
With stem cell therapies finally reaching the clinical trial stage, however, one has to wonder whether citizens really do distinguish between specific clinical applications based on the types of stem cells used. After all, as Nisbet and Lewenstein have shown, news coverage of biotechnology tends to focus overwhelmingly on scientific “Progress” and the potential benefits of specific breakthroughs, so it’s possible that any ethical concerns that loom large in the abstract might fall by the wayside when people think about a specific stem cell therapy.
So does the public in fact care whether a given therapy uses adult or iPS cells instead of embryonic stem cells? The short answer: Yes, but only under certain conditions.
In an interesting study, Stewart and colleagues found that when people were presented with a news story about regenerative medicine that used a “scientific progress” frame, they did not differentiate between adult and embryonic stem cells. When the story featured a “political conflict” frame, though, they tended to view adult stem cells as the more ethical of the two. In other words, the type of stem cells used in a specific regenerative medicine application only appears to become a salient consideration for the public when the communications environment focuses people’s attention on the issue. [pullquote]…the type of stem cells used in a specific regenerative medicine application only appears to become a salient consideration for the public when the communications environment focuses people’s attention on the issue.”[/pullquote]The perceived benefits of stem cell applications also have a strong impact on how much people care about the type of stem cells used. In a recent study published in Nature Biotechnology, for example, Evans and Kelley investigated Americans’ attitudes towards a range of different applications of stem cell technology. As I’ve written about elsewhere, one of their key findings is that Americans strongly support stem cell therapies to treat serious diseases like heart disease and cancer, regardless of whether iPSCs or embryonic stem cells are used. So it looks like when the potential benefits of a regenerative medicine application are high, people’s concern about embryonic research plays a secondary role in determining their attitudes, which may help to explain why U.S. voters have supported a more permissive regulatory environment for stem cell research in several state-level ballot initiatives.
One problem with these studies, though, is that they ask the same individuals to evaluate the different types of stem cell therapies, which may draw their attention to the differences between them, and lead them to explicitly compare the different proposed applications based on the source of the stem cells used. So even these conditional results may be overstating the extent to which citizens distinguish between different stem cell therapies based on type of cells they use.
To test this in a different way, Edna Einsiedel and I explored this question in a recent Stem Cell Network-funded survey of Canadian adults by using an experimental approach. Our 1,231 respondents were each randomly assigned to read one of six versions of a simulated Globe and Mail article reporting on a new stem cell therapy for age-related macular degeneration (AMD).
For one third of our sample, the therapy was described as using iPSCs, while the other two thirds of participants read articles in which the stem cells were produced using two therapeutic cloning methods: somatic cell nuclear transfer (SCNT) and interspecies SCNT (iSCNT). SCNT-derived cells are different than traditional embryonic stem cells in that they are taken from a cloned embryo that shares the patient’s DNA and was created specifically for the therapy, rather than from a “left-over” embryo that would otherwise have been discarded, but they still prompt the same ethical concerns about embryonic research. This experimental design, then, allowed us to infer that any differences in support for the therapy across the experimental conditions were actually the result of the process used to generate the stem cells.
We also included a separate manipulation in which half of the sample read versions of the article in which opponents of the therapy concluded their argument by describing the stem cells used in the treatment as “unnatural.” This way of framing opposition to new biotechnologies – which we might refer to as the “unnaturalness objection” – is a widely-used technique through which anti-biotechnology activists are able to raise moral questions about specific biotechnological applications without necessarily specifying what is wrong with them. We expected this objection to focus people’s attention on their ethical concerns about the way in which the stem cells used in the therapy were generated.
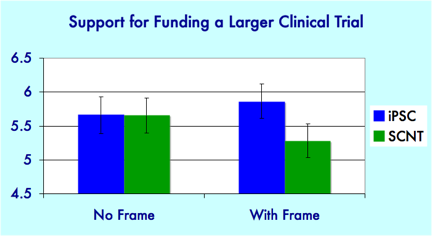
So what did we find? The chart below shows the expected level of support for the idea that “[t]he federal government should fund a larger clinical trial of this treatment for macular degeneration.” We used a 7-point scale ranging from “Strongly Disagree” at 1 to “Strongly Agree” at 7 to measure support.
Overall, our sample was supportive of funding a larger trial, with all the expected values falling over the neutral midpoint of the scale (4). As you can see, though, there were significant differences in support for a larger trial across the experimental conditions.
When the simulated news article focused on evaluating the potential benefits and risks of the therapy in question (No Frame), participants were as likely to support funding an iPSC-based therapy as one that involved SCNT. When opponents described the stem cells as “unnatural” (With Frame), however, participants were significantly more likely to support funding for a larger trial of the iPSC-based therapy than for a therapy that used SCNT-derived stem cells. Interestingly, this pattern held even among the subgroup of respondents who believed that embryos had the same moral status as a person.[pullquote]When the research is framed primarily in terms of scientific progress…individuals don’t seem to take the source of the stem cells into account.”[/pullquote]In short, our experiment largely confirms the findings in previous research. Citizens do sometimes judge specific stem cell therapies based on the process used to generate the stem cells, but only when the issue is framed in moral terms. When the research is framed primarily in terms of scientific progress and the potential benefits it might bring to society, individuals don’t seem to take the source of the stem cells into account.
So what lessons can regenerative medicine advocates and researchers draw from these results and from the broader literature? I’d say there are at least three:
- It’s clear that iPSCs really are less controversial than stem cells derived from embryos. Citizens do not distinguish between these types of stem cells in a typical science communication context, but when the issue is framed in moral terms (which opponents of embryonic research tend to do), a public preference for iPSCs does emerge.
- As a result, if and when iPSCs and adult stem cells become the principal tools of regenerative medicine, the social controversy over stem cell research is likely to wane.
- In the meantime, regenerative medicine advocates are probably best served by continuing to focus on communicating the potential social benefits of stem cell research.
Latest posts by Nick Dragojlovic (see all)
- The race to develop senescent cell clearance therapies - May 3, 2016
- How online outreach adds value to scientific research - March 4, 2015
- Update on crowdfunding in the regenerative medicine space - May 26, 2014






Trackbacks/Pingbacks